It’s been a solid month since my last post. Everything really caught up with me after the stem cell transplant on Feb. 7. I lost interest in pretty much doing anything except getting through the process and recovery. The transplant itself went quite well. They wheel my frozen (-175 degrees C) stem cells into the room on this cart and then thaw them out. 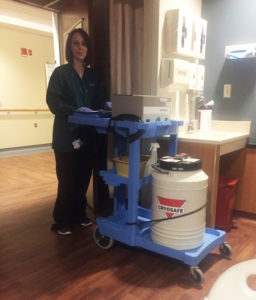 The Chaplain blessed them for me. I figured since I was baptized at birth I didn’t want the new stem cells to feel left out. And Feb. 7 is my new birthday! Then it was simply a matter of hanging an IV bag for about 45 minutes. Altogether there were six people in the room plus Jill and me. Of the six, five of them grew up within ten miles of our home in Novi, Livonia, Farmington, or Farmington Hills. Certainly an interesting coincidence, but it likely stems from that mass exodus of young college graduates from around southeastern Michigan when there were no jobs to be found.
The Chaplain blessed them for me. I figured since I was baptized at birth I didn’t want the new stem cells to feel left out. And Feb. 7 is my new birthday! Then it was simply a matter of hanging an IV bag for about 45 minutes. Altogether there were six people in the room plus Jill and me. Of the six, five of them grew up within ten miles of our home in Novi, Livonia, Farmington, or Farmington Hills. Certainly an interesting coincidence, but it likely stems from that mass exodus of young college graduates from around southeastern Michigan when there were no jobs to be found.
All of the build up and the chemotherapy leading up to the actual transplant had me so tense that the actual transplant procedure was somewhat anti-climactic. Just very relieved  to have reached that milestone with no major problems so I was exhausted the rest of the day. On Day +1 I received my last dose of Rituxan. I was not yet neutropenic, which is a requirement in a successful stem cell transplant. However, my white blood cell counts and neutrophil counts were still dropping. Neutropenia occurs when they are essentially near zero (<0.1). On Day +2 I had perhaps the only significant hiccup in the whole process when my heart rate jumped to 162 bpm (supra-venticular tachycardia) and then a couple of hours later I went into atrial fibrillation.
to have reached that milestone with no major problems so I was exhausted the rest of the day. On Day +1 I received my last dose of Rituxan. I was not yet neutropenic, which is a requirement in a successful stem cell transplant. However, my white blood cell counts and neutrophil counts were still dropping. Neutropenia occurs when they are essentially near zero (<0.1). On Day +2 I had perhaps the only significant hiccup in the whole process when my heart rate jumped to 162 bpm (supra-venticular tachycardia) and then a couple of hours later I went into atrial fibrillation.
Under normal circumstances I would be transferred to the cardiac ICU where they can better deal with these events. However, that meant moving me off the stem cell floor where infection control is paramount and the air is HEPA filtered to prevent possible infections to patients with no immune systems. I was not enthusiastic about going anywhere. In the end, the medical team decided to keep me where I was and try to reduce the heart rate with medication. If that did not work, I was going elsewhere. After six hours or so my heart rate was down to acceptable limits (<100 bpm) which relieved me no end. From Day +3 to when I was discharged on Day +11 it was simply a waiting game. The big event each day was seeing what my blood lab results were. I did not become neutropenic until Day +5 when both the neutrophil and white blood cell counts dropped to essentially zero. I stayed there for five days, at which time they finally began to rise again.
Dr. Burt did say that the delay in reaching a neutropenic state is a result of using the “heart friendly” protocol. Under the standard protocol most patients become neutropenic around Day 0, but this is a more gradual slope. Same result, but not as drastic a drop in blood levels. Given my episode with SVT and A-fib, I suspect that had I gone through the standard protocol I might now be a statistic or at least had a much rougher go of it. (Thank you, Dr. Burt!)
Following transplant, I was incredibly weak. The typical response when doctors ask “How do you feel today?” is “I feel like I got run over by a truck.” And I was no exception. This derives from the chemotherapy and the transplant process, the atrial fibrillation where my heart is not pumping efficiently, and just the deconditioning that takes place from lying in bed for weeks on end. I’m now at Day +25 and just beginning to be able to get through a day without collapsing on the couch for hours at a time. The other not-so-fun side effect is what they refer to as chemo-brain, which is the fog I seem to be in all the time. I took several books with me because I figured I would have more time to read than I had ever had. However, linear thinking where I want to put several thoughts together became very difficult. I would just forget what I was trying to say. And reading for any length of time I found taxing. For the most part, I was a couch potato and now very well versed in virtually all episodes of Blue Bloods and NCIS. This chemo-brain will disappear over the next 2-3 months, so if I seem somewhat more eccentric than usual, it’s not dementia. Or at least that’s my story and I’m sticking to it!

Dave, I’m glad everything seems to be going so well and is reassuring to see you back online. I have that same kind of brain fog some days I call it Lupie brain, and then some days just fine. I’ve been thinking of you a lot and praying and hoping the best for you and Jill. You are quite a warrior and I admire your courage and fortitude!
Dave, thinking about you and praying everyday!! Hang tough!
Thanks for the update. You are amazing.
Dave,
I have been wondering how your journey was progressing. So damn glad the grill was the only thing that got you!!!😜 Sounds like a wild ride….glad you held on tight! Prayers for smoother roads ahead🤗😘
Proud of you Dave… blessing to have Jill! Thuy and I have you in our prayers and look forward to sitting in the sun with in Dexter… do what you’ve always done… keep those feet moving! 🙂
Cousin Dave,
Wow, what a ride! Sounds as if you have peeled your face off that grill, now in the driver’s seat. Blessings to you and Jill as you continue to be in our prayers. Keep that positive Kurtz attitude!
Great picture of you and your Dad.
So relieved to hear from you. Surely you cannot be “foggy”sending such an articulate
account of your progress. The foggy stuff comes when you are eighty plus!!!
My thoughts and prayers are with you and Jill, Dave, and my love,as well..Aunt Dixie
Glad to see the update Dave. I took note of your new birthday and plan on sending you greetings when Feb 7 rolls around again.
Once the fog clears you’ll be a Democrat like the rest of us. Best.
Once the fog clears Rush Limbaugh is going to sound like a moderate…
Dave,
Glad to hear that you are doing well and congratulations on being born-again. You have been in our thoughts and prayers continuously. We are counting on your progress to continue and we look forward to a spring or summer reunion at which time we may have to uncork a good bottle of wine or two to celebrate. In the meantime, Mia and I send our love to you and Jill. Keep up the good fight brother!
With warmest personal regards,
Stan and Mia Materka
Dave I did not know that you were having medical issues. I am glad that you are doing well My experiences with chemo-brain is the foggynes took 3-4 months for the feeling to fully go away. Hopefully it will take you less time to recover.
Get well and stay that way little brother